Tag Archives: plaque
Move to create common diagnosis for Alzheimer’s
 Paris: Two studies to help establish an internationally consistent approach to detecting Alzheimer’s disease have been reported at the Alzheimer’s Association International Conference 2011 in Paris.
Paris: Two studies to help establish an internationally consistent approach to detecting Alzheimer’s disease have been reported at the Alzheimer’s Association International Conference 2011 in Paris.
The research, focusing on biomarkers – telltale biological indicators of Alzheimer’s – could help standardise the detection of the disease and increase the accuracy of clinical trials by ensuring those most likely to benefit from drugs or preventions take part.
The first study examined the association between a well-established Alzheimer’s risk gene – APOE4 – age, and a hallmark protein in Alzheimer’s – amyloid – to test the consistency of the relationship across ethnic groups. Led by researchers from Japan, the study took data from three different national populations – the US, Australia and Japan – all three of which include people with Alzheimer’s, mild cognitive impairment and normal individuals.
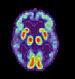
The team evaluated the influence of the APOE4 risk gene and age on the build up of amyloid in the brain, measured by PET scans. Amongst the three populations, the researchers observed consistency in the way amyloid build-up was affected by the risk gene and age, showing the biomarkers to be consistent across different ethnic groups – crucial for a test to be internationally applicable.
A second study concentrated on the hippocampus, responsible for the formation of new memories and usually the first area of the brain to be affected by Alzheimer’s. MRI scans have become increasingly important in tracking shrinkage in this area of the brain, which can be useful for diagnosis and measuring disease progress.
Researchers in Italy have been examining and compiling the different approaches to MRI scanning used in worldwide dementia research to measuring volume changes in the hippocampus. The team’s next step is to review the different approaches and draw on the input of an international panel of experts to determine a common protocol.
Dr Simon Ridley, Head of Research at the UK‘s leading dementia research charity, Alzheimer’s Research UK, said: “If we are to effectively test new treatments or preventions, we have to be able detect Alzheimer’s early to get people involved in trials who stand to benefit most. An approach to detection that works consistently across the world is crucial to the global effort to defeat dementia and work towards that goal is to be welcomed.
“Numbers or people living with dementia are spiralling towards a million in the UK alone; research is the only answer to defeating the condition. Investment across all areas of dementia research – diagnosis, prevention and treatment – is urgently needed”.
More Information about Alzheimer’s Research UK
• Alzheimer’s Research UK is the UK’s leading charity specialising in finding preventions, treatments and a cure for dementia
• To help us defeat dementia, donate today by visiting www.alzheimersresearchuk.org or calling 01223 843899
• We are currently supporting dementia research projects worth £17 million in leading Universities across the UK
• The Alzheimer’s Association International Conference (AAIC) is the world’s largest conference of its kind, bringing together researchers from around the world to report and discuss groundbreaking research and information on the cause, diagnosis, treatment and prevention of Alzheimer’s disease and related disorders
• Ref: Kenji Ishii, MD; et al. Age, APOE ε4, and Ethnic Effect on [C-11]PiB in Multi-national ADNI Studies – Direct Comparison of J-ADNI, US-ADNI and AIBL Data
• Ref: Giovanni Frisoni, MD; et al. Estimating the Impact of Differences among Protocols for Manual Hippocampal Segmentation on Alzheimer’s Disease-Related Atrophy: Preparatory Phase for a Harmonized Protocol.
Vitamin D and curcumin could get rid of Alzheimer plaque
Los Angeles: Vitamin D and curcumin could help rid the brain of Alzheimer’s plaques, according to scientists at the University of California Riverside and Los Angeles.
They have found that a combination of vitamin D3 and a synthetic form of curcumin could help remove amyloid beta from the brains of Alzheimers disease patients. The research was published in the July, 2009 issue of the Journal of Alzheimer’s Disease.
Amyloid beta accumulates in the brain when the innate immune system fails to clear it. The substance forms the plaques that, along with neurofibrillary tangles, characterize Alzheimers disease. For their research, Dr Milan Fiala of UCLAs David Geffen School of Medicine and his associates tested the effects vitamin D and curcuminoids, which are synthetic forms of the compound curcumin, on white blood cells known as monocytes derived from nine men and women with Alzheimers disease, one man with mild cognitive impairment, and three control subjects. Monocytes are immune system cells that transform into macrophages which travel through the body to consume waste products, including amyloid beta.
The team found that vitamin D3 significantly stimulated phagocytosis and clearance of amyloid beta while protecting against programmed cell death. Specific curcuminoids increased amyloid beta clearance by enhancing its surface binding to macrophages.
Synthetic forms of curcumin were tested in the current experiments due to challenges with natural curcumins ability to absorb and remain stable. Nevertheless, previous research conducted by the team found that not all Alzheimers disease patients respond to curcuminoids.
“We hope that vitamin D3 and curcumin, both naturally occurring nutrients, may offer new preventive and treatment possibilities for Alzheimer’s disease,” stated Dr Fiala. “Since vitamin D and curcumin work differently with the immune system, we may find that a combination of the two or each used alone may be more effective depending on the individual patient.”
Try the finest quality vitamin D at www.vitalityshopuk.com
Scientists develop early-warning plaque detector

Liverpool: Scientists at the University of Liverpool have developed a new dental product to identify plaque build-up in the mouth before it is visible to the human eye.
The toothbrush-sized product has a blue light at its tip, which, when shone around the mouth and viewed through yellow glasses with a red filter, allows plaque to be seen easily as a red glow. The device, produced in collaboration with dental and healthcare developers, Inspektor Research Systems BV, has been designed for everyday use in the home.
Dentists currently use disclosing agents in tablet form to uncover tooth decay and plaque but these often stain the mouth and taste unpleasant. The new product, known as Inspektor TC, will be particularly useful for those who are vulnerable to dental diseases such as children and the elderly.
Children in the UK have had an average of 2.5 teeth filled or removed by the age of 15 because of tooth decay. In young people alone £45 million is currently being spent every year on the problem.
Professor Sue Higham, from the Universitys School of Dental Sciences, said: It is extremely difficult to get rid of all plaque in the mouth. Left undisturbed it becomes what we call mature plaque and gets thicker. This is what leads to gingivitis, or bleeding gums, and decay.
Early stage plaque is invisible, and so this device will show people the parts of the mouth that they are neglecting when they brush their teeth, enabling them to remove plaque before it becomes a problem.
Inspektor TC is designed so that people can easily incorporate it into their daily dental hygiene routine at home. We now hope to work with industry partners to develop this prototype so that people can use it in the home to identify plaque before any serious dental work is needed.
The team has now received a Medical Futures Innovation Award for the product a commendation which acknowledges significant innovation in science.
More information
1. Inspektor Research Systems BV is an industrial collaborator based in Norway which focuses on research and analysis to develop innovative dental and healthcare products.
2. Medical Futures Innovation Awards recognise groundbreaking ideas and products within the healthcare and business world that have the potential to transform peoples lives. Past winners of the award have secured over £80 million of funding from industry specialists for the manufacture of their product.
3. The University of Liverpool is a member of the Russell Group of leading research-intensive institutions in the UK. It attracts collaborative and contract research commissions from a wide range of national and international organisations valued at more than £93 million annually.
ALZHEIMER’S DISEASE
Blood pressure drugs help cut Alzheimer’s risk
Chicago: Drugs used to cut blood pressure has been shown to improve the risk of Alzheimer’s.
According to a new US study of angiotensin receptor blockers, or ARBs, which are normally prescribed as a second choice treatment to patients unable to tolerate ACE inhibitors, another class of blood pressure drug, the results are dramatic.
Both drugs work by allowing the blood vessels to the vessels to relax and widen so more blood can flow through them, which cuts blood pressure.
Alzheimer’s is associated with high blood pressure, damaged arteries and amaloid plaques, a type of protein which attaches itself to the neurotransmitters in the brain.
In the new study, an Alzheimer’s conference in Chicago was told, six million patients treated for high blood pressure between 2001 and 2006 were examined by scientists.
Those taking ARBs were 35 to 40 per cent less likely to develop Alzheimer’s or other forms of dementia than patients on other medications.
Patients already suffering from Alzheimer’s when they started taking ARBs had a 45 per cent reduced chance of developing delirium, being admitted to a nursing home, or dying prematurely during the period of the study.
Those who had experienced strokes before or during the course of their illness appeared to benefit most from the drugs.
Study leader Professor Benjamin Wolozin, of Boston university medical school, said: ‘For those who already have dementia, use of ARBs might delay deterioration of brain function and help keep patients out of nursing homes. The study is particularly interesting because we compared the effects of ARBs to other medications used for treating blood pressure or cardiovascular disease.’
Alzheimer’s Disease is affecting more and more older adults as people live longer.
Can tomatoes fight Alzheimer’s?

Seol: Korean scientists have genetically modified tomatoes to produce a prototype vacinne against Alzheimer’s Disease.
The disease, kills brain cells when a sticky plaque known as beta-amyloid protein clogs up nerve connections.
And the disease, which starts with short-term memory loss and leads to death, is on the increase as people live longer.Current drugs do not prevent or cure it but only slow its progress.
The researchers from the Korea Research Institute of Bioscience and Biotechnology say they have genetically modified the fruit to create an edible vaccine that fires up the immune system to fight the disease.
To create the vaccine, the scientists combined the gene behind the beta-amyloid protein with the tomato’s genetic code.They then used mice to experiment with the designer tomatoes.
Blood samples taken from the mice revealed the tomatoes triggered their immune systems to release disease-fighting antibodies, although the levels of plaques in the brain were not reduced.
They said the tomato was a good way of getting a vaccine into the body because it was enjoyable to eat and could be eaten raw.The vaccine could be destroyed if the tomatoes were cooked, they added.
Tomatoes are already known as a natural antioxidant. They cut cholesterol and may help prevent some cancers (prostate, rectal and colon), protect against sunburn and are packed with vitamin C. The active ingredient is called lycopene which is responsible for the red colour.
Intelligent hide mental decline, US survey reveals

New York: Highly educated people are better at hiding the signs of dementia which means they go downhill faster in the later stages of Alzheimer’s, says a new report from the Albert Einstein College of Medicine of Yeshiva University.
Alzheimer’s is caused by an accumulation of ‘plaques and tangles’ or protein deposits in the brain which may first lead to difficulty finding words. This progresses to typical symptoms of dementia, loss of memory, confusion and agitation.
Researchers in New York at looked at 117 people who developed dementia out of an original group of 488 from the 1980s onwards.
The study looked at people born between 1894 and 1908, had formal education levels ranging from less than three years’ schooling to postgraduate level. For six years, they were given annual cognitive tests which assessed memory, speech and ability to think.
The results, published in the journal Neurology, found that for each additional year of formal education, the accelerated memory decline associated with oncoming dementia was delayed by approximately two and a half months.
However, once that rapid decline commenced, those with more education saw their rate of decline accelerate 4 per cent faster for each additional year of education.
They found that, for example, a college graduate with 16 years of education, whose dementia is diagnosed at age 85, would have begun to experience accelerated memory decline 3.8 years earlier, at age 81.
A person with just four years of education, who is diagnosed at the same age, would have begun to experience a less rapid rate of decline around age 79, more than six years before diagnosis.
Researcher Charles Hall, an associate professor at Albert Einstein College, said it was well recognised that intelligent dementia victims get symptoms at a later stage than less clever sufferers.
‘Our study showed that a person with 16 years of formal education would experience a rate of memory decline that is 50 per cent faster than someone with just four years education,’ he said.
‘This rapid decline may be explained by how people with more education have a greater cognitive reserve, or the brain’s ability to maintain function in spite of damage.
‘So, while they’re often diagnosed with dementia at a later date – which we believe may be because of their ability to hide the symptoms – there’s still damage to their brain.’
Dr Hall said the better educated did not make a ‘conscious’ effort to hide their failing memory, but were benefiting from greater mental reserves which allowed them to compensate for it in the short-term.
He added that the fact that highly- educated dementia victims experience a period of rapid mental decline will have implications for the families and for the success of new treatments.
Scientists create cells that disolve Alzheimer’s plaque
Genetically engineered cells, that produce an enzyme that disolves the toxic plaques associated with Alzheimers disease, have been produced by scientists.
The researchers used mice which they infected with a human gene that caused them to develop, at an accelerated rate, the disease that robs millions of elderly people of their memories. After receiving the doctored cells, the brain-muddling plaques melted away. If this works in humans, old age could be a much happier time of life.
Alzheimers involves a protein called amyloid-beta, which makes up gooey clots or plaques that form in the brain. These toxic clumps, along with accessory tangled fibers, kill brain cells and interfere with memory and thinking. The situation has been compared to a build-up of cholesterol in coronary arteries.
Delivery of genes that led to production of an enzyme that breaks up amyloid showed robust clearance of plaques in the brains of the mice, notes Dennis Selkoe, Vincent and Stella Coates Professor of Neurologic Diseases at Harvard Medical School. These results support and encourage further investigation of gene therapy for treatment of this common and devastating disease in humans.
The first published report of the experiments, done by Selkoe and other researchers from Harvard-affiliated Brigham and Womens and McLean hospitals, appeared Aug. 27 on the Web site of the Public Library of Science.
The gene delivery technique employed by the research team has been used in several other trials with animals that model human diseases, including cancers. The procedure involves removing cells from patients, making genetic changes, and then putting back the modified cells, which should treat a disease or disability. So far, this approach has produced encouraging results for cancers, blood, muscle, and eye diseases, spinal cord injuries, stroke, Parkinsons and Huntington diseases, and amyotrophic lateral sclerosis (Lou Gehrigs disease). Several of these potential treatments have advanced to human trials, with encouraging outcomes for patients, says Matthew Hemming, lead author of the report and a graduate student in Selkoes lab.
Another way to do gene therapy involves using a virus to carry the curative gene to target cells. However, two people have died and three contracted leukemia in experiments using this method. The drawback of using viruses this way is that the added gene often mixes with the patients genome in ways that can lead to unwanted side effects, including cancer and, possibly, death.
The Harvard team used skin cells from the animals own body to introduce a gene for an amyloid-busting enzyme known as neprilysin. The skin cells, also known as fibroblasts, do not form tumors or move from the implantation site, Hemming notes. They cause no detectable adverse side effects and can easily be taken from a patients skin. In addition, other genes can be added to the fibroblast-neprilysin combo, which will eliminate the implants if something starts to go wrong.
Will it work in humans?
This method worked well in the Alzheimer’s experiments. The gene that removed the amyloid-beta may not only prevent brain cells from dying, but will also remove the toxic protein that drives the disease progression, Hemming comments.
The experiments proved that the technique works, but will it work in humans? One major obstacle, Selkoe says, is the larger size of a human brain compared to that of a mouse. That difference will require an increase of amyloid-busting activity throughout a much larger space.
One solution might involve implanting the genes and fibroblasts where they have the best access to amyloid-beta, in the spinal fluid for example, instead of trying to inject them into a small target. The amyloid-killing combo might be put into capsules that would secrete neprilysin into the blood circulating in the brain, eliminating the need to hit an exact spot.
This or some other clever maneuver that does not require surgery might eliminate the gooey plaques, but will that improve a persons memory? And will the change be long-lasting? Further work is needed to determine if reducing the plaque burden has cognitive benefits over a long period, notes Hemming, but theres a wealth of evidence arguing that it will.
More information at www.news.harvard.edu
Statins may be new weapon against Alzheimer’s
Seattle: The family of anti-cholesterol drugs called statins and taken by millions around the world, can protect against Alzheimer’s disease, according to new research.
An examination of brain tissue has provided the first direct evidence that statins – taken to prevent heart disease and strokes – can also ward off dementia and memory loss. The study is published in the American Journal of Neurology.
The new findings s come from a study of 110 brains – donated for medical research – at the University of Washington School of Medicine in Seattle. The researchers led by Dr Gail Li examined the brains for changes linked to Alzheimer’s -including the creation of ‘plaques’ and ‘tangles’ made from the protein called beta amyloid.
These changes appear in the brain long before any symptoms of dementia develop. Eventually, they damage enough brain cells to trigger confusion, memory loss and eventually death. The researchers found far fewer tangles in the brains of people who had taken statins, compared to those who had not.
The findings were true even after age, sex and the history of strokes were taken into account. This is the first study to compare the brains of people who took statins with those who did not.
Dr Eric Larson, study co-author said: “These results are exciting, novel and have important implications for prevention strategies.”
Statins work by blocking the action of a chemical in the liver which is needed to make the ‘bad’ form of cholesterol, LDL. Reducing levels of bad cholesterol keeps blood vessels unclogged.
The researchers are not sure how statins also prevent the buildup of protein tangles in the brain. They suspect that a healthy flow of blood is a key factor.
Another study, five year’s ago at Boston University found that statins may cut the risk of Alzheimer’s by as much as 79 per cent, even in people with a family history of the disease. Some small- scale studies have found an apparent link between statins and cancer and Parkinson’s disease. Other studies, however, suggest that the drugs can ease the pain of rheumatoid arthritis.